
Neurofeedback for ADHD: What the Research Says
Neurofeedback for ADHD: What the Research Says
ADHD affects an estimated 3 to 5 percent of children and around 2 percent of adults in the UK. The standard treatment pathway involves medication, behavioural strategies, or both. But a growing number of families and adults are asking whether neurofeedback might offer an alternative or complementary approach. Here, we look at what the research actually says, honestly and without overclaiming.
ADHD and the Brain
ADHD is a neurodevelopmental condition rooted in how the brain develops and functions. Research using EEG has consistently found that individuals with ADHD show characteristic brainwave patterns, most notably an elevated theta-to-beta ratio. This means relatively more slow-wave (theta) activity and less fast-wave (beta) activity than expected, particularly over the frontal regions responsible for executive function, planning, and impulse control.
This does not mean the brain is "broken." It means the brain's electrical regulation is different, manifesting as difficulties with sustained attention, impulsivity, and task completion. Understanding ADHD at this level reframes the conversation from willpower to neurology.
ADHD is not a lack of intelligence or effort. It is a difference in how the brain regulates its electrical activity, and that difference can be measured and, research suggests, trained.
How Neurofeedback Addresses ADHD
The principle behind using neurofeedback for ADHD is straightforward. If the brain is producing too much slow-wave activity and not enough fast-wave activity in the regions responsible for attention and executive function, we can train the brain to shift that balance.
During a session, sensors on the scalp monitor brainwave activity in real time. When the brain produces the desired pattern, the client receives a reward through a film or game. When the brain drifts back, the reward pauses. Over many sessions, the brain learns to sustain the more regulated pattern independently.
The most common protocols for ADHD include:
- Theta/beta ratio training: Reducing theta and increasing beta over the frontal cortex
- Sensorimotor rhythm (SMR) training: Enhancing activity in the 12-15 Hz range, associated with calm focus and reduced impulsivity
- Slow cortical potential (SCP) training: Training the brain's ability to shift between states of activation and deactivation
At our clinic, the specific protocol is always guided by an initial brain map (QEEG), which identifies the individual's unique pattern rather than applying a one-size-fits-all approach.
The Research Evidence
Neurofeedback for ADHD is one of the most extensively researched applications of this technology. The evidence has evolved considerably over the past two decades.
Meta-Analyses and Large-Scale Reviews
A landmark meta-analysis by Arns et al. (2009) in Clinical EEG and Neuroscience reviewed 15 studies and found large effect sizes for inattention and impulsivity, comparable to stimulant medication. An updated analysis (Arns et al., 2020) confirmed these findings and noted that improvements in attention were maintained at follow-up, suggesting neurofeedback may produce lasting changes rather than effects that disappear when treatment stops.
Randomised Controlled Trials
The study by Strehl et al. (2017) in European Child and Adolescent Psychiatry showed significant improvements in parent-rated and teacher-rated attention for children receiving neurofeedback versus a sham condition. The Collaborative Neurofeedback Group's study (Arnold et al., 2021), one of the largest double-blind trials to date, found significant parent-rated improvements and neurophysiological changes in the neurofeedback group.
American Academy of Pediatrics Rating
In 2012, the American Academy of Pediatrics (AAP) updated its evidence-based child and adolescent psychosocial interventions evaluation, rating neurofeedback as a Level 1 "Best Support" intervention for ADHD. This is the highest level of evidence classification, placing it alongside well-established treatments.
A Balanced View
While the overall trend is positive, the quality of blinding varies across studies. When only the most rigorously blinded studies are considered, effect sizes tend to be smaller, though still meaningful. The consensus is moving towards recognising neurofeedback as a promising intervention for ADHD, while acknowledging that further sham-controlled research would strengthen the evidence.
NICE Guidelines Context
In the UK, the National Institute for Health and Care Excellence (NICE) provides clinical guidelines for ADHD management. As of the most recent guidelines, NICE does not specifically recommend neurofeedback as a first-line treatment for ADHD. The guidelines focus primarily on medication (methylphenidate, lisdexamfetamine) and behavioural interventions.
However, NICE guidelines are updated periodically and do not preclude the use of other evidence-informed interventions. Many families choose neurofeedback alongside conventional approaches, particularly when medication has not been well tolerated or has produced unwanted side effects.
Children vs Adults
The majority of neurofeedback research for ADHD has been conducted with children and adolescents, which is where the evidence base is strongest. Our children and young people programme is specifically designed to make sessions engaging and age-appropriate for younger clients.
That said, a growing number of studies are examining neurofeedback in adults with ADHD, with encouraging results. Adults often present with different challenges: organisation, time management, emotional regulation, and maintaining focus professionally. Research by Mayer et al. (2016) and Schonenberg et al. (2017) found improvements in attention and executive function in adult populations.
Our ADHD and Focus programme is designed for both children and adults, with protocols adapted to the individual's age, presentation, and brain map findings.
What to Expect from a Programme
If you are considering neurofeedback for ADHD, here is a realistic picture of what a programme typically involves:
- Initial assessment: A comprehensive QEEG brain map to identify your specific brainwave patterns and confirm which protocol is most appropriate.
- Training programme: A typical course involves 30 to 40 sessions, usually two to three times per week. Consistency is important for building new neural pathways.
- Early changes: Many clients and families report noticing initial improvements in focus and behaviour within the first 10 to 15 sessions. These early changes can be subtle and are sometimes first noticed by teachers or family members.
- Consolidation: The later sessions consolidate the gains and help ensure they are maintained over time.
- Follow-up: A repeat brain map at the end of training allows us to objectively measure changes in brainwave patterns and compare them to the baseline.
Results vary from person to person. Research suggests that approximately 60 to 75 percent of individuals with ADHD show meaningful improvement with neurofeedback. Those who respond well often describe better sustained attention, reduced impulsivity, improved emotional regulation, and a greater sense of calm.
Combining Approaches
Neurofeedback does not need to be an either/or decision. Many of our clients use it alongside other approaches:
- Medication: Neurofeedback can be used alongside ADHD medication. Some clients find they can reduce their dosage in consultation with their prescribing clinician.
- Behavioural strategies: Neurofeedback addresses the underlying neurology while behavioural strategies provide practical daily tools. The two complement each other well.
- Therapy: Combining neurofeedback with counselling or CBT can address both neurological and psychological dimensions.
- Lifestyle factors: Sleep, exercise, nutrition, and screen time all influence brain function and form part of a holistic approach.
The goal of neurofeedback for ADHD is not to eliminate who you are. It is to give your brain the tools to regulate itself more effectively, so you can access your full potential with less struggle.
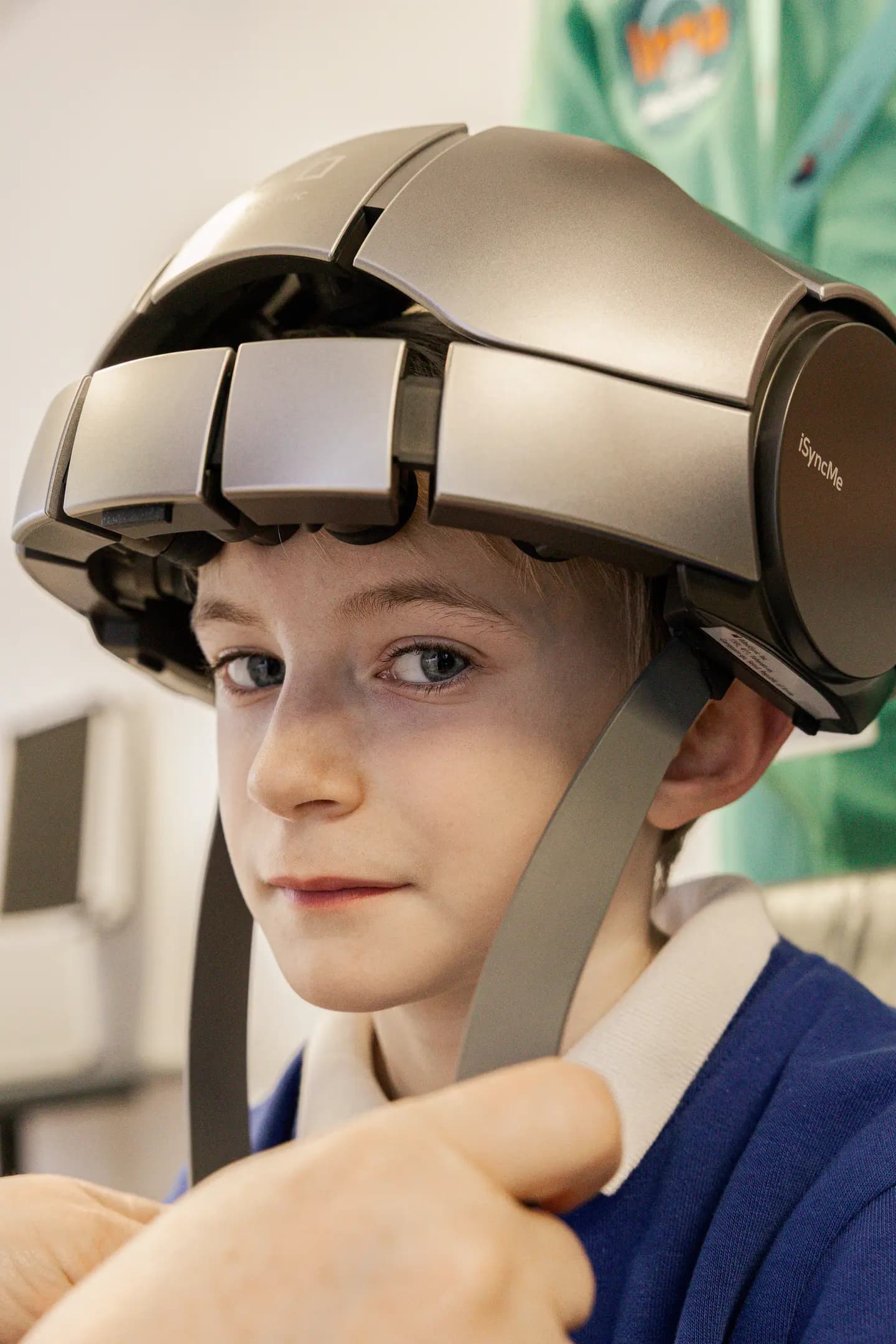
At Inna MediSync, neurofeedback for ADHD is often complemented by Photobiomodulation (PBM Care) sessions using the iSyncMe device. PBM Care uses near-infrared light to support cellular energy production in the brain, which may help enhance the results of neurofeedback training. Both protocols are delivered in separate, dedicated sessions and can be combined as part of a personalised neurotherapy plan.
Take the Next Step
If you or your child has been diagnosed with ADHD, or if you suspect ADHD may be playing a role in daily difficulties, neurofeedback may be worth exploring. Our ADHD and Focus programme at Inna MediSync combines a thorough brain map assessment with a personalised training plan designed around your individual needs. Based in Romford, Essex, we welcome clients from across London. Get in touch to arrange a no-obligation conversation with one of our practitioners.
Inna MediSync Clinical Team
Neurotherapy Specialists
The Inna MediSync clinical team brings together certified neurotherapy practitioners with expertise in QEEG brain mapping and neurofeedback. Every article is reviewed for clinical accuracy and reflects our commitment to evidence-informed practice.
Continue Reading
Ready to Explore Neurotherapy?
Take the first step towards understanding your brain. Book a free consultation with our clinical team.

